“Diabetic Retinopathy” is one of the symptoms that diabetic patients must be cautious of because it carries a high risk of causing blindness if they do not take good care of their eye health.
So how do diabetic patients know if they are at risk of blindness? What are the symptoms of diabetic retinopathy? What causes it? How can it be prevented and treated? You can study this information to take care of yourself or diabetic patients.
Diabetic Retinopathy
- Understanding Diabetic Retinopathy
-
-
- How many stages does diabetic retinopathy have?
-
- Warning signs! Symptoms of diabetic retinopathy to watch out for
- What causes diabetic retinopathy?
- Guidelines for preventing diabetic retinopathy
- Treatment of diabetic retinopathy
- Frequently asked questions about diabetic retinopathy symptoms
-
-
- Is diabetic retinopathy dangerous?
- When should diabetic patients have their eyes checked?
- Can diabetic retinopathy be cured?
- What can diabetic retinopathy patients eat?
-
Did you know! Diabetic patients who have had the disease for more than 10 years have over an 80% chance of developing diabetic retinopathy
Diabetic retinopathy is a complication in diabetic patients who cannot control their blood sugar levels within a safe range. Prolonged high blood sugar causes sugar to block the blood vessels in the retina, preventing normal blood flow. The capillary walls deteriorate throughout the body, including the retinal vessels, causing inflammation, swelling, bleeding, and fluid leakage in the retina.
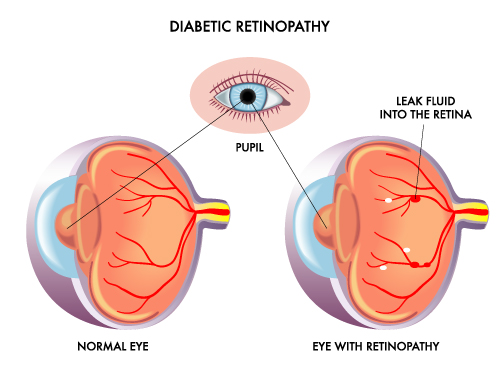
When inflammation begins, patients often do not realize it. If patients neglect eye health check-ups as recommended by doctors, they usually become aware only when symptoms worsen. This may cause blurred vision because the inflammation reaches the central point of vision. If left untreated, it can cause retinal tears and detachment, leading to vision loss or complete blindness.
How many stages does diabetic retinopathy have?
1. Non-proliferative Diabetic Retinopathy (NPDR)
This is the early stage where patients usually do not feel any abnormalities. Eye exams may reveal retinal hemorrhages and leakage of fluid from blood vessels, causing retinal swelling and mild blurred vision. However, if the macula is swollen (macular edema) or there is ischemia, it can lead to vision loss.
2. Proliferative Diabetic Retinopathy (PDR)
This is a more severe stage where new blood vessels (neovascularization) form due to severe ischemia. These new vessels are fragile and prone to bleeding into the vitreous, causing fibrous tissue formation that pulls on the retina. At this stage, patients often experience significant vision loss and may suffer permanent blindness.
If the new vessels interfere with the drainage of aqueous humor from the eye, it can increase intraocular pressure, damaging the optic nerve that transmits images from the eye to the brain, potentially causing glaucoma.
Warning signs! Symptoms of diabetic retinopathy to watch out for
In the early stages of diabetic retinopathy, patients may not notice any symptoms. Therefore, blurred vision indicates advanced diabetic retinopathy, and patients should promptly see an ophthalmologist for an eye exam.
Urgent symptoms of diabetic retinopathy that require immediate medical attention include:
- Blurred vision, worsening eyesight, unstable vision
- Seeing black spots or cobweb-like lines floating
- Distorted images
- Difficulty distinguishing colors
- Dark bands in the field of vision
- Progressive vision loss leading to blindness
What causes diabetic retinopathy?
Diabetic retinopathy is caused by prolonged high blood sugar levels, which can result from several factors such as:
- Duration of diabetes (the longer the disease, the higher the risk)
- Poor blood sugar control, often due to dietary habits
- High blood pressure and high blood lipids
- Smoking or pregnancy, among others
Guidelines for preventing diabetic retinopathy
The best prevention is to reduce the risk of developing diabetes. For those who already have diabetes, it is important to prevent and reduce the risk of diabetic complications by following these steps:
- Choose nutritious foods and reduce salty, sweet, and high-fat foods
- Exercise regularly and maintain a healthy weight
- Quit smoking and avoid alcohol consumption
- Take diabetes medications as prescribed by the doctor
- Keep blood sugar levels within the normal range (between 70-100 mg/dL)
- Control blood pressure; diabetic patients should keep blood pressure below 140/90 mmHg
- Control blood lipid levels; diabetic patients should maintain normal lipid levels
- Monitor changes in vision; if sudden changes such as blurred vision, unclear sight, or black spots occur, see a doctor immediately
- Have regular annual eye exams with an ophthalmologist, even if there are no vision problems
Treatment of diabetic retinopathy
How is diabetic retinopathy treated? Initially, if the patient is in the early stage, the doctor will advise controlling blood sugar levels within the normal range and managing other underlying conditions such as hypertension and kidney disease appropriately to slow disease progression.
If symptoms worsen, there are currently three treatment methods for diabetic retinopathy:
- Laser treatment for diabetic retinopathy
Laser treatment is the standard treatment for patients diagnosed with proliferative diabetic retinopathy or macular edema. Laser therapy helps shrink abnormal new blood vessels, reduces retinal swelling, prevents bleeding in the eye, and slows progression to blindness.
- Medication treatment for diabetic retinopathy
Medication treatment involves injecting drugs into the vitreous humor. These drugs reduce blood vessel leakage and shrink new blood vessels. The treatment is effective but the drug’s effect is temporary and there is a risk of complications from the injection, such as inflammation or vitreous hemorrhage.
- Surgical treatment for diabetic retinopathy
Surgery is performed for severe cases with extensive vitreous hemorrhage and fibrous tissue pulling on the retina. Vitrectomy surgery helps prevent disease progression and can repair retinal detachment, reducing the risk of blindness. However, vision may not fully recover depending on the severity of the disease in each patient.
Frequently Asked Questions about Diabetic Retinopathy
Is diabetic retinopathy dangerous?
Diabetic retinopathy is a dangerous complication because it can lead to complete blindness if neglected or if diabetes is not well controlled. Patients who allow their blood sugar to remain high for a long time and do not receive proper and continuous treatment are at risk.
Additionally, prolonged high blood sugar can cause other severe complications such as kidney failure, cardiovascular disease, or even limb amputation.
When should diabetic patients have their eyes checked?
All diabetic patients should have their eyes examined by an ophthalmologist and follow up at least once a year. Early detection allows for appropriate prevention and treatment.
Can diabetic retinopathy be cured?
Diabetic retinopathy cannot be completely reversed to normal. Treatment focuses on preventing disease progression or worsening by controlling blood sugar and HbA1c levels within normal limits.
What can diabetic retinopathy patients eat?
Diet control to prevent high blood sugar involves choosing nutritious foods, focusing on healthy eating, and reducing salty, sweet, and high-fat foods.
- Recommended to eat lean meats or low-fat meats such as fish and chicken breast
- Eat fruits that are not very sweet, such as guava, apple, rose apple, and orange
- Avoid sweets and foods high in sugar (e.g., thong yip, thong yod, foi thong)
- Avoid adding extra seasoning such as salt, fish sauce, light soy sauce, and sauces
In summary, diabetic retinopathy can be prevented by controlling blood sugar levels within the normal range and having regular annual eye exams to reduce the risk of severe complications. If diabetic retinopathy occurs, early treatment to prevent progression is crucial. Neglecting high blood sugar and not receiving proper treatment can lead to severe diabetic retinopathy and complete blindness.
Dr. Suwanna Chaichumsak
Endocrinologist and Metabolism Specialist
Diabetes and Endocrine Center


